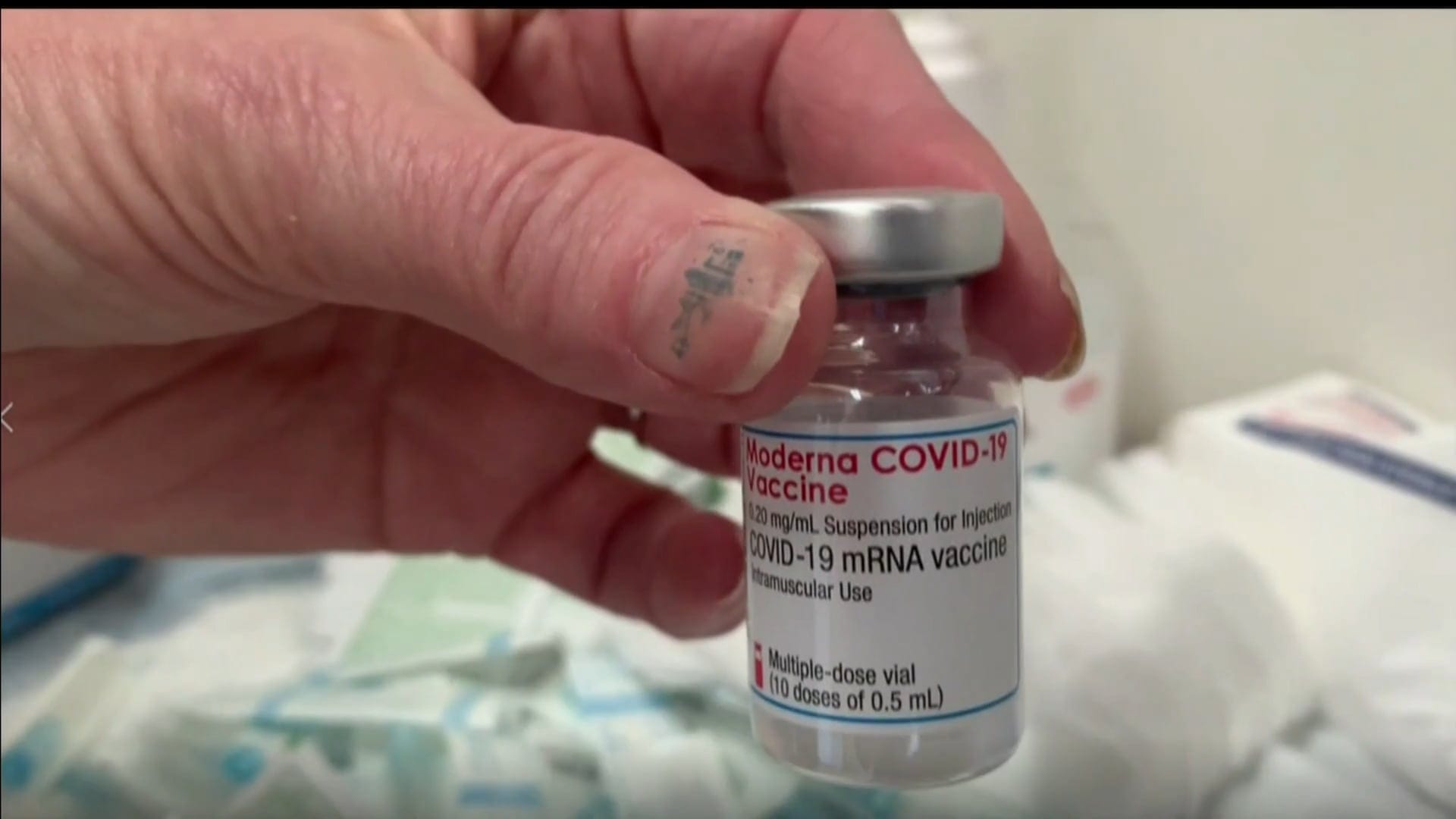
Many First Nations across the country used checkpoints and lockdowns to keep the novel coronavirus out of their communities as cases spiked elsewhere. Photo: APTN
When Ms. Bourque finally arrived home in Edmonton from Atikameg (Whitefish Lake) First Nation, about a four-hour drive northwest of the city, she was greeted by a mean-looking stray cat perched on the curtain rod in the living room.
The tomcat had slipped in through the pet door and taken up residence in Bourque’s home during the six weeks she was in Atikameg leading the community’s COVID-19 response as the nurse in charge.
After the cat scurried out of her house and things had settled down, Bourque enjoyed the first moment of relaxation she’d had for weeks.
She was only given the chance to return home to isolate because she was considered a contact of someone who had tested positive for COVID-19.
When the community’s first known case was discovered on Oct. 23, Bourque’s hard work began.
She often spent 12 or more hours in the office. Nurses from the First Nations and Inuit Health Branch (FNIB) arrived to help a few days later, as did nurses from a neighbouring reserve, but even with reinforcements the hours were long, she said.
When the nurses left by the end of the month, Bourque said she was on her own again, with one nurse helping to contact trace for about three weeks. Paramedics from the First Nation began assisting her in early November.
“When we were (in a) full blown outbreak here, I was working every night until nine. I was so tired I could hardly keep my eyes open,” she said.
At some points during the pandemic response she said she broke down crying.
After enjoying her moment of rest in Edmonton, Bourque retrieved her laptop and multiple work phones from her car. They were some of her closest companions throughout the pandemic. Then, she sat down and waited for the phones to ring, as they always did.
There were 116 confirmed cases in Atikameg before the first outbreak was finally resolved in early March. But then on April 13 four more residents tested positive, pushing the community into a second wave. As of June 26, there had been a total of 141, though everyone was finally recovered.
During the first six months of the pandemic, First Nation communities in Canada virtually avoided the virus. Indigenous Services Canada (ISC) recorded 425 total COVID-19 cases in the second week of August, 383 of which had recovered.
By the first week of November, total cases had risen to nearly 2,300, only about 1,300 of which had recovered.
For those communities located far from cities, the isolation seemed to be enough to keep them out of harm’s way. But that changed as the pandemic dragged on.
Many First Nation leaders blame longstanding issues that haven’t been addressed.
Using registered First Nation population data and total case numbers pulled from the ISC webpage, APTN News calculated approximate case rates in First Nation communities.
While rates remain below those in the general population in Ontario and eastward, it’s a different matter in the west.
We found that by late June, the rate of total COVID-19 cases per 100,000 people was between 1.7 and 2.3 times higher in First Nations communities in the western provinces than in the population of those provinces as a whole.
As of June 22, the rate of known active cases of COVID-19 in First Nation communities across Canada are six times the rate of the general population, according to ISC.
At the end of 2020, cases began to soar in western First Nations, and that continued into early 2021 before weekly case numbers dropped somewhat and stabilized at an average of 465 a week from May 2 to June 19, according to ISC data. Cases in the general population have dropped more steeply in recent weeks, however.
It’s not in dispute that First Nation communities have a lack of healthcare resources, high rates of food insecurity, inadequate water access and poorer living conditions that are overcrowded. Medical experts, advocacy organizations and the Canadian government have referenced these inequities when discussing high case rates in these communities.
The National Advisory Committee on Immunization, which advises the Public Health Agency of Canada, said that Indigenous communities have been prioritized for vaccines because they have been disproportionately impacted by past pandemics, may have reduced access to health care and “infection could have disproportionate consequences.”
The government’s choice to prioritize Indigenous people has led to racist remarks questioning their position in the vaccine rollout plans.
“As I’ve spoken to this before, the decision to prioritize Indigenous people … is based on science, not a matter of politics or opinions,” Indigenous Services Minister Marc Miller said in February.
ISC said it hopes to have all Indigenous adults vaccinated by the summer.
Miller said in an interview in May that uptake has been positive and he is optimistic that they can meet that goal.
As of June 25, vaccinations were underway in about 687 First Nation communities with a little more than 614,000 doses having been administered. About 40 per cent of those are second doses in people 12 and older.
APTN attempted to contact ISC to determine how many doses it would take to fully vaccinate all communities, but did not receive a response.
When looking at COVID-19 between early January and late June, the disparity of case rates in the Western provinces—the gaps in the rate of total cases in First Nation communities and the general population—peaked between early March and late April, before narrowing.
The narrowing was partly because of a springtime surge of cases in the general population. Experts suggest First Nations were largely spared that surge because of widespread vaccination.
ISC admits that less access to healthcare and a lack of infrastructure—including housing, medical services, and a clean water supply—creates or worsens the risk for First Nations people.
In fact, Miller said Indigenous communities are three-and-a-half to five times more likely to be impacted by COVID-19 than non-Indigenous communities.
It makes sense. It’s hard to isolate in a house crowded with people, to wash your hands when there’s no clean water available or to stay healthy without access to nutritious food or healthcare resources.
“The reasons for that are well-documented and, frankly, entirely unacceptable,” Miller said.
Ottawa has announced more than $4.2 billion in assistance for Indigenous and northern communities and organizations to combat COVID-19, outside of the 2021 federal budget.
It’s an attempt to catch up to the issues that have been affecting Indigenous communities for decades, and that have been exacerbated by COVID-19 and its effects. But, how badly has COVID-19 affected Indigenous Peoples living in First Nation communities, and how do we know?
APTN has been collecting the COVID-19 data posted by ISC nearly every day since early January to determine how First Nation communities in Western Canada have been affected by the COVID-19.
By using the case data from ISC, and federal data of registered First Nations populations as of February 2021, APTN calculated the approximate rate of total cases per 100,000 First Nation people living in on-reserve communities.
When we compared with the overall provincial data from provinces in Western Canada, rates of total cases were significantly worse in First Nation communities—but that’s not surprising for some. First Nation community leaders and experts saw this coming.
“When this first started, we said it’s going to be devastating for First Nations in the long run because of overcrowding and the lack of houses in the community,” said David Monias, chief of Pimicikamak Cree Nation in northern Manitoba during a press conference on Feb. 16. “We’ve been stating this for a long time.”
Pimickamak Cree Nation, also known as Cross Lake Cree Nation, located about 520 km north of Winnipeg, declared a state of emergency on March 16, 2020. Monias said the community closed its borders to outsiders and took a serious approach to the pandemic—closing schools, care homes, pubs, and neighbourhoods with enforced check stops.
The novel coronavirus still impacted a large portion of their community. There are about 6,300 people registered with thee community living on-reserve according to government data. About 700 people were infected, which is about 11 per cent of their on-reserve population, leading to 11 deaths, according to community officials.
It’s been one of the worst affected First Nation communities in Manitoba.
Monias said their once close-knit community that was once abundant in celebrations—concerts, sports, cookouts—had been relegated to their homes. It dampened their spirits. Regulations were as specific as set shopping schedules to ensure a store doesn’t exceed capacity.
Officials said some regulations, like the shopping schedules, have since lifted, but a curfew and the border closures are still in place.
Monias said all these changes altered how he led his community.
“It’s a lot of working in terms of protection, a person’s physical safety, emotional safety, and mental safety. Where before it used to be more about community development and building on the nation—protecting lands and waters and so forth,” he said.
Unfortunately, medical attention isn’t always available to those who need it in remote reserve communities. People infected with COVID-19, or close contacts of positive cases, are often sent to Winnipeg, Monias said.
The school was set up as an isolation accommodation, since schools and daycares were shutdown due to the pandemic and because isolating in the home has been problematic.
A lot of people, too few homes
Like other First Nation communities in Canada, there are poor living conditions in Pimicikamak, including overcrowded housing.
While there are exceptions, the general standard for a household is that each adult should have their own room, according to the National Occupancy Standard, and there shouldn’t be more than two children to a bedroom.
In Pimicikamak, Monias said it’s common for multiple families to be living in a single home. He estimates there are about a dozen people in each. In an extreme case there were nearly 40 people in a single home.
“You would have a problem in terms of isolating, or in terms of social distance and you only have one washroom to a family of, say, 25 living in a household.”
Monias said there are about 1,200 homes in the Pimicikamak Nation region, hundreds of which have been affected.
He said that Pimicikamak made an application for about 100 houses under the Rapid Housing Initiative, a $1 billion program to address housing needs of vulnerable Canadians during the pandemic. Monias said the community needs more than 100 homes (he estimates the number is nearer 1,000) but he was just hoping for a positive response to his request.
According to the community’s housing director, the application wasn’t approved and they weren’t informed why.
George Muswaggon grew up in Pimicikamak.
He lives outside of the community but works on reserve. Like others in the community, he has taken on a few roles during the pandemic out of necessity. Some days he’s an office administrator, others a COVID-19 patient transporter. Muswaggon said overcrowded housing is a significant issue in the community.
“There’s nowhere you can stand in Cross Lake where you will not visually and personally see … multiple family units. In fact, most of the houses are multiple family units,” he said.
“The house across from where I live, I think there’s eight or nine individuals in that house—individuals who were infected by COVID-19. A stone’s throw from that house, there was a household of 26 people of which 20 of them tested positive, including the children.”
The impact of the pandemic on First Nation communities in Canada has been largely attributed to the overcrowded and inadequate living accommodations by government, experts, and community members. Homes on reserve have long been plagued by issues with mold and poor conditions, or too many occupants, or both.
In Fisher River Cree Nation, located about 177 km north of Winnipeg, there have been 120 confirmed cases and, as of June 26, there was one active case remaining.
Like Pimicikamak Nation, Chief David Crate said he locked down the community early in the pandemic, including checkpoints and curfews. Despite their restrictions, the community’s first case was travel-related, brought in by someone returning from Winnipeg.
Crate said that they’ve had no water issues, and that while the community needs about 250 homes, it’s not in dire straits.
“Compared to some of the northern communities, where they have eight to 10 people residing in a home, just because of housing shortages … we have that problem here, but it’s not on a large scale,” Crate said, explaining they don’t have large families that contribute to overcrowding, as other communities do.
When isolating at home wasn’t an option, there were sometimes alternative isolation accommodations that have been developed through partnerships or provincial planning. In Fisher River, when community members needed to isolate there was a motel outfitted for the purpose.
In other communities, there are other forms of alternative isolation spaces, including accommodations in urban centers. It’s a development that has aided some community response, but it is not always completely effective.
Delays in testing, or identifying contacts, means people can often be exposed to others for several days before arrangements for alternative isolation are made. In some situations, people won’t accept alternative accommodations.
Housing has foundational issues
Al Isfeld, an Ojibway retired carpenter, spent his construction career in and out of First Nation communities in Ontario and Manitoba.
“Every time we went to the reserve, housing [was] an issue,” he said. “They’re always behind, they’re always trying to catch up, in every community. I’ve never, ever been to a First Nations community that had adequate housing.”
In Western Canada, where more than half of First Nations people reside in Canada and where there are the highest rates of infection in First Nation communities, overcrowded housing has been an issue for decades.
It starts with land ownership. Legally, reserve lands are considered Crown lands which the Indian Act said are “set aside for the use and benefit” of band members but are owned by the federal government. That Indian Act provision means that while First Nations Peoples can live in the home, the ground its on is owned by the Crown, which makes housing a federal responsibility.
Even after a shift in 1996 that allowed more First Nation sovereignty and control under the On-Reserve Housing Policy, housing management remains in disarray, and homes in disrepair. Even now there’s still debate about which entity—the community, CMHC or the federal government—controls particular aspects of housing in First Nation communities, such as construction and upkeep.
Several evaluations and reports of on-reserve housing have been conducted since the shift to the current approach in 1996, most recently in 2017, each with recommendations such as developing stronger mandates and simplifying funding. But inadequate housing and overcrowding is still a major concern in many communities.
The evaluation of on-reserve homes published by the former Department of Indigenous and Northern Affairs Canada in 2017, showed that Alberta, Saskatchewan and Manitoba had the highest rate of people living in overcrowded homes from 2001 to 2011.
The evaluation documented the link between poor housing conditions and the spread of infectious disease. It listed the prairie provinces as some of the most vulnerable, alongside Ontario.
According to the evaluation, an average of about one in five people on reserve in the prairie provinces lived in an overcrowded home. To be more specific, a 2015 Senate report stated there were about 8.4 people per home in Saskatchewan.
Officials in all of the four communities APTN spoke to said they had issues with overcrowding, to varying degrees.
When too many people are living in a home, it deteriorates more quickly. Isfeld said things such as poor construction or materials (and how they’re stored) could affect durability.
After the houses are built, poor maintenance or the inability for moisture-control measures to keep up to an excess of people in a home—whether it’s bathing, or cooking, or just living—puts strain on the structure.
Houses can’t be built quickly enough to keep up with the number of houses falling into disarray. When a new house is built, Isfeld said it’s doomed from the start because with so many inadequate homes, the new ones become overcrowded—and the cycle starts again.
Each year, about $280 million is put toward housing in First Nation on-reserve communities—a little more than half through the Canada Mortgage and Housing Corporation, and the rest via other government of Canada agencies.
Funds are earmarked for renovations and new homes, among other supports like training and shelters for victims of domestic violence.
The 2017 report conducted for on-reserve housing found that current proposal-based funding brought short-term successes to First Nation communities, but was considered “short-sighted and non-strategic.”
“There’s going to be another crisis down the road after, and … it’s all going to lead back to the same thing. It’s all going to lead back to the people been living in squalor, and people living in houses that are overcrowded and living conditions where there isn’t enough housing,” Isfeld said.
“Until you address that, don’t be expect anything to be any different than it is.”
It’s a two-steps-forward, one step back approach to the problem that has created poor living conditions and cramped spaces that are ideal for viral transmission. The evaluation report of on-reserve homes recognized it, and so do experts, doctors and medical health officers.
That includes Dr. Nnamdi Ndubuka, the medical health officer for the Northern Inter-Tribal Health Authority (NITHA) in Saskatchewan, which serves about 26,000 people living on reserves in the province’s north.
Ndubuka said the high rate of infection has a lot to do with social determinants of health, which are social and economic factors that influence a person’s health and wellbeing. Main determinants can include elements such as income, education or childhood experiences.
In some Indigenous communities, though, it’s the physical environments, and access to necessities such as food, clean water and health services.
“The determinants of health continued to impact the health of Indigenous people way before the pandemic—the pandemic only brought it to the fore,” he said.
Joint data analysis between the ISC and the NITHA found that as of late December 2020, First Nation residents over the age of 40, per capita, have been hospitalized at three times the rate of the general population in Saskatchewan, within their respective age groups, Ndubuka said.
It also showed that First Nation people living on reserve have a COVID-19 mortality rate three times higher than the general population in the province.
More infections, fewer deaths
While First Nation communities have had higher rates of COVID-19 than the general population in Western Canada, most communities have reported fewer deaths per capita than the general population.
“Currently, what we’re looking at is the mortality rate is only a fraction of Canada(‘s),” said Miller. “But that is only because Indigenous communities have reacted with such seriousness in terms of taking measures related to tracking, tracing, and isolation, public health measures, getting the vaccine out early.”
In Manitoba, where the First Nations Health and Social Secretariat of Manitoba diligently tracks pandemic data, deaths both on- and off-reserve are low.
Indigenous people make up almost one in every three of the total cases of COVID-19 in the province, the secretariat says, and only one in every five deaths is an Indigenous person.
While the mortality rate for those infected in Manitoba is about two per cent, the rate on reserve is about one per cent, according to data from the Manitoba secretariat.
Dr. Evan Adams, deputy chief medical officer at ISC, speculates that the disparity between case counts and fatalities is because of which ages are being affected.
“In other Canadians, COVID has affected older populations and we have much younger populations with fewer older people—and also our infections have tended to be in younger people who experience mild illness, compared to other Canadians,” Adams said.
“That might be, in part, because we’ve been focusing vaccinations on older people, than on younger people. It also just might be that younger people have a harder time self-isolating or limiting their contact than older people.”
In Manitoba, deaths in long-term care homes make up more than 40 per cent of Manitoba’s COVID-19 fatalities, according to government data and long-term care data from the National Institute on Ageing which has been tracking COVID-19 in care homes.
According to the Manitoba secretariat, the median age for deaths is more than 15 years younger in First Nation communities.
Vulnerability, not susceptibility
In an interview with Dr. Malcom King, a public health professor at Simon Fraser University and the University of Saskatchewan, I had asked why First Nation people could be more susceptible to the virus—drawing from ISC’s assertion that Indigenous people are at higher risk.
King corrected me. He said that higher rates of infection is not a biological issue, the distinction is that First Nation people are more vulnerable to the virus, not more susceptible to it.
“There’s this perception that First Nation people have a susceptibility to diabetes,” King said. “Well, there’s actually a very minor genetic component that might account for 10 or 15 per cent of the excess diabetes that it’s other factors related to nutrition, related to poverty.
“Susceptibility, to me, is a sort of misleading word because it somehow implies that: so sad, too bad, First Nation people are going to get sick more, as opposed to the underlying reasons.
“Why you have these higher rates (of infection is) not because of some genetic issue but because of social and systemic factors, primarily—and only to a minor extent, if at all, to genetic conditions.”
But, King believes there may also be another aspect, beyond the determinants of health, affecting Indigenous health outcomes: epigenetic effects.
The stressors, he explains, cause deep-rooted changes in the body and how it reacts. He referenced the Second World War and the Nazi occupation of the Netherlands, where the population was starving. Children born in the last few months of the occupation had lifelong health deficits, like heart problems, but those born before and immediately after the war did not.
“It’s very definitely this period of biological stress that their mothers (experienced) when pregnant—and grossly underfed, undernourished, had suffered—and it continued really through the lifetime of these Dutch people,” he said. “The residential schools, other aspects of trauma, have the same kind of effect.”
Epigenetics don’t change the genetics of a person, but stressors like residential schools, poverty, or displacement especially if they’re repeated or ongoing, could alter how the genes create proteins in the body.
“So, there is a good explanation for all of this and it has nothing to do with inherent susceptibility, but everything to do with traumas—repeated and ongoing traumas, and interacting traumas even,” King said.
King believes isolation was one of the strongest defenses for some of these First Nation communities. In northern Saskatchewan, it was a major defence; and once that wall fell, Covid spread quickly.
A lack of basic necessities
Ndubuka said people travelling to larger urban centres introduced isolated communities to the virus—travelling for things such as medical care, recreational trips or to other First Nation communities. Precautionary travel restrictions were imposed, but not always followed.
First Nation communities also face inadequate water access, which limits their ability to follow public recommendations such as consistent handwashing.
The federal government promised to deliver accessible, clean drinking water to every First Nation community in Canada, but delayed that promise in late 2020.
As of June 16, the most recent update on water advisories in First Nation communities, there were 51 long-term water advisories in effect across 32 communities in Canada, the majority of which are in Ontario.
As of June 24, there were 29 short-term advisories in First Nation communities.
Dr. Lalita Bharadwaj, a health and epidemiology professor at the University of Saskatchewan who researches water and health in First Nation communities, said it’s difficult to draw a direct correlation between how water access may have affected COVID-19 infection rates, but agrees limited water access could create hygienic challenges.
Bharadwaj said that determining if there’s a link between water access and COVID-19 infections would take a large-scale study that included all of the more than 600 communities in Canada.
Dr. Marcia Anderson, the public health lead of the Manitoba First Nation Pandemic Response Coordination Team, and the lead medical officer of health for ISC in Manitoba, has been a key component in the vaccine rollout in Manitoba.
She also said that alongside housing issues, COVID-19 outbreaks can be influenced by food insecurity or nutrition and a lack of healthcare resources in First Nation communities.
“People who are food insecure are actually more likely to have underlying chronic diseases … (and) certainly when we are more well-nourished with a well-balanced diet, our immune systems are going to function better,” Anderson said.
The Assembly of First Nations (AFN), University of Ottawa and University of Montréal conducted a First Nations food, nutrition and environment study between 2008 and 2018 to understand how well communities are eating, and if the food and water are safe to consume.
In Manitoba, nine First Nation communities were part of a one of those studies in 2010, including Pimicikamak. The study found that, on average, it cost Manitoba First Nation communities $100 more to feed a family of four, per week, than urban communities.
It also found that nearly two in five households experienced food insecurity. About one-third of people worried their food would run out before they could buy more.
Similar studies from the project were done in Alberta, in 2013 with 10 communities, and Saskatchewan, in 2015 with 14 communities. In Alberta, nearly half of households were food insecure, and 37 per cent in Saskatchewan.
While Anderson said food distribution programs have been a “key initiative” in several communities, she’s aware of people having to break isolation in order to get access to food.
But, high COVID-19 infection rates aren’t only affecting Indigenous people in rural First Nation communities.
While the federal government has kept national data on infections in reserve communities, there hasn’t been national data publicized about Covid-19 cases of people who have status under the Indian Act and are living off reserve.
“Sometimes people mistakenly think that things are worse on reserve. And it’s important that folks know that off-reserve Indigenous people also experience challenges with housing, with food, and income, and security, and with inequitable access to health care,” Anderson said.
“We have consistently seen off-reserve First Nations (individuals) have, at least, the same risk when it comes to Covid-19 and slightly higher risk actually when it comes to experiencing severe outcomes.”
Mapping outbreaks in Winnipeg
Using community area and 2016 census Aboriginal population data drawn from the City of Winnipeg, and COVID-19 data from the Manitoba government, APTN constructed maps that show the proportion of Indigenous people in community areas, and the rate of COVID-19 in those areas.
APTN attempted to look at other cities, such as Edmonton or Calgary, but there wasn’t sufficient data.
These maps show the population density of Indigenous people in Winnipeg community areas, in blue, and the rates of COVID-19 per 100,000 people, in red.
According to City of Winnipeg data, the Indigenous population is highest in the Point Douglas, Downtown and River East community areas. COVID-19 infection rates were highest in the Downtown and Point Douglas communities.
“Throughout the second wave, which was kind of, you know, fall (and) early winter, we actually saw higher rates in Winnipeg than we did in First Nation communities on reserve,” Anderson said.
A race to vaccinate
Anderson, the public health lead for the First Nation pandemic response team is concerned that another wave, including a wider spread of COVID-19 variants, could further impact Indigenous people, especially at younger ages.
“Our median ages for severe outcomes are 15 to 20 years younger than (in) the general population. And so that’s what concerns me,” Anderson said.
According to the health and social secretariat, the median age of death in First Nation people is 63, compared to 81 in the overall Manitoba population.
As of June 24, about three in four people on-reserve in Manitoba had received one dose, and nearly half had received two doses.
It’s a race: complete vaccinations before the virus spreads. Anderson’s experience with pandemics, and this one in particular, led her to believe another wave with the COVID-19 variants will continue to exploit issues such as overcrowded housing, and continue to impact First Nation communities.
“Non-crowded housing I would say is more exceptional than crowded housing is,” she said. “We have frequently had cases where during the contact tracing or the case investigation process, the number of people in a two- or three-bedroom home is consistently, I would say, six, eight, and into the twenties.”
Anderson said the first phase of vaccinations was well-accepted. Now, she said, communities are seeing more variation in uptake, and young people have appeared to be the most resistant to getting vaccinated.
In the general population, some have been skeptical of the vaccine because of how quickly it was developed, or issues involving the AstraZeneca vaccine which has caused rare blood clots in recipients.
Anderson has been doing her best to inform First Nation communities that they will receive the Moderna vaccine, rather than the AstraZeneca. All First Nation communities in Canada have either been receiving the Pfizer or Moderna vaccines.
Misinformation on social media has also been a factor.
Anderson said she’s found younger people are less likely to show up for the vaccine, and Bourque has said she’s seen the same young age groups express skepticism online.
“I find the older people like, you know, 50 and up, ask a lot of questions and they research and they find out for themselves. The ones that don’t research just completely downright refuse it,” Bourque said of her experience.
“I find in the younger people, they’re believing a lot (of misinformation) and they’re not researching—like teenagers and the 20 (to) 30-year-olds. You know, I see online posts that say, “Why are we being forced to take a [needle?].”
In the general population, it’s tough to keep up with the constant influx of information. In First Nation communities, it’s complicated by access and translation.
In Atikameg, Bourque wants more information in Cree, specifically for the variants of concern. In Pimicikamak, George Muswaggon said he helps translate messages, but finds some of the information is lost in translation.
There have been examples of translation helping inform people, especially Elders, in First Nation communities and encouraging vaccine uptake.
Avoiding another pandemic spread

While vaccines roll out to First Nation communities across Canada, the socioeconomic reasons that brought Indigenous people to the front of vaccine lines remain.
When asked if another virus like COVID-19 could affect Indigenous people similarly if these structural issues weren’t addressed, Adams didn’t provide a definitive answer.
“Definitely, one can say, Indigenous peoples are more prone to some infectious diseases, and some chronic diseases, because of their social situations,” said Adams.
Ndubuka, the medical officer in Saskatchewan’s northern health authority, said there needs to be policy changes to discontinue the cycle of housing issues that have opened the door to widespread COVID-19 infections.
Leah Gazan, member of Parliament for Winnipeg Centre, is disappointed with the government’s COVID-19 support given to Indigenous communities.
“It’s as a result of actual leadership within the First Nations communities that we’ve been able to manage the pandemic as well as we have in spite of these ongoing and grotesque human rights violations that are perpetrated against First Nations communities, historically and in an ongoing basis,” she said.
“First Nations communities … received less than one per cent of the overall COVID support—even though Indigenous people comprise five per cent of the total Canadian population—which is appalling.”
In an interview, Miller called her claim “inaccurate.”
When asked what kind of policies need to be put in place, or what recommendations she had for the federal government, Gazan didn’t provide specific examples but said the government needs to produce and publish a plan to end boil water advisories and provide “these minimum human rights (such as) access to clean drinking water.”
In response, Miller said he acknowledged that these necessities are missing and that the budget allotment of $18 billion over five years is a “significant percentage … invested towards that important relationship.”
Those billions, about 18 per cent of the budget amount, is meant to “narrow gaps between Indigenous and non-Indigenous peoples.”
On May 26, the Office of the Auditor General of Canada released a report detailing ISC’s response to requests for additional PPE and nurse staffing.
According to the report, about 963 requests were made for extra contract nurses and paramedics to assist communities’ pandemic response. Of those, ISC didn’t meet a little more than half of those requests, which meant some communities weren’t able to access proper health services during the pandemic.
As for personal protective equipment, the report found weaknesses in the department’s storage and allocation, but found it adapted quickly to respond to the pandemic.
The ISC agreed to the two recommendations set out by the report, which include reviewing their PPE management and working with isolated communities to address the nurse shortage as well as review best health practices.
Several issues have contributed to the affect the pandemic has had on First Nation communities, but housing is at the centre as a common factor for food insecurity and the spread of disease. Sources vary in how many homes are needed to address the housing crisis in First Nation communities.
An evaluation by the former Department of Indigenous and Northern Affairs Canada puts the number in a broad range from 20,000 to as many as 87,000.
The AFN, a national group that advocates for and represents First Nation Peoples in Canada, estimates there will be a backlog of 130,000 units by 2031, which could take several decades to fill at the current rate of investment, according to the 2015 Senate report.
If the Canadian government wants to fix the housing issues in First Nation communities it will have to contribute billions of additional dollars to a solution.
The Senate report estimated cost it could take between $3 billion and $5 billion to eliminate the housing deficit, although in a press conference in mid-May, Miller said that he wasn’t sure of the exact cost but that “number seems low.”
Of the money set aside in the budget for supporting Indigenous communities, $6 billion has been tagged for addressing infrastructure gaps over the next five years, such as establishing adequate access to clean water, housing, schools and roads.
The amount directed specifically toward housing hasn’t been determined. Miller said that this budget won’t fill the gaps but will be a step closer to doing so.
What’s next?
Miller said ISC is rolling out a plan to communicate with First Nation communities over the next year or two to see which infrastructure gaps need filling—ranging from roads to schools and from housing to hospitals.
When asked what kind of assurance the government could provide in meeting that goal—after recently failing to end long-term water advisories by 2020 as promised.
“Promises have been made in the past and broken,” he said. “Throughout this pandemic we have taken—very importantly, for the results that it has yielded— clear steps to engage with communities that make sure that they have the financial backing of the Government of Canada to do what they know best to do, which is protect their own peoples.”
He referenced the Rapid Housing Initiative which supplied homes to Indigenous communities, among others. He said while it filled an “important part” of the need, there is still much of the need that remains “unfilled.”
While Miller said the department is working with communities, some have argued that they want to be more involved in the making of these decisions.
Marlene Poitras, the regional chief for the AFN in Alberta, has seen the commitments the government has made over the past year as a strong effort. In spite of infrastructure issues, the financial backing helped Indigenous communities—but she doesn’t think the First Nation Peoples are as involved in decisions as they should be.
“There’s been chronic housing shortages, lack of drinking water (and) we still have a lot of boil-water advisories in the communities. It’s just poor-quality access to health services, systemic racism that exists within the healthcare system, I mean those are deep, foundational issues that need to be addressed,” said Poitras.
In terms of housing, she said, First Nation people are “the experts, we know what the issues are. It’s been a long time coming, but First Nations need to be at the table.”
In Saskatchewan, Miller and the leader of the First Nations Capital and Infrastructure Agency of Saskatchewan—a First Nations-led organization—recently signed an agreement that “sets a path” to allow the Agency to independently deliver housing and infrastructure services to communities.
Kim Beaudin, vice-chief of the Congress of Aboriginal Peoples (CAP) which represents Indigenous people who live in urban centres, said the people they and the people they represent have been ignored. He also wants to pull up a chair to these decisions.
“I can tell you that the federal government came up with the largest budget allotment in its history (for Indigenous peoples) and there was really no money allocated for Indigenous people living off-reserve,” he said.
He said that the federal government doesn’t recognize the congress for distinctions-based programs, which is a funding model used for different initiatives.
CAP said it examined this year’s budget. In an email, it outlined the amount it determined it was eligible for in this year’s budget, which was under $1 billion, but that doesn’t mean it would receive all of it. CAP said off-reserve Indigenous peoples would be competing for that funding with on-reserve peoples. It doesn’t expect to receive much.
Beaudin said it feels like Indigenous people living off-reserve don’t exist.
“The lion’s share of the budget went to reserves and bands and things. I don’t have a problem with that … because I don’t even think it’s enough for people living on-reserve either,” Beaudin said.
In May, the government said they allocated $30 million to “increase Indigenous Peoples’ access to traditional and nutritious foods” through the Indigenous Community Support Fund.
The money was allocated largely to Western Canada, as well as national organizations, including $3 million to CAP.
King, the public health professor, said that whatever policies or changes are made to address these issues, they need to holistically address Indigenous wellness, something Miller agreed with and said that the holistic approach has been a key component of the pandemic response, and has yielded better outcomes in Indigenous communities.
“I’m not saying don’t also deal with improving health services and health service delivery, but really to look at health and wellness more broadly, it’s a factor that depends not only on health services but also on things like identity, education, language and so on,” King said.
The AFN wants a rights-based approach to housing with more autonomy across all aspects of housing, including band-owned, individual ownership and social housing. That includes potentially setting up a First Nation-managed entity to oversee accessible funding.
Al Isfeld, the retired Ojibway carpenter, has specific ideas on how he thinks the federal government can resolve the housing issue.
He said he wants a feasibility study done in each community, handled by the community, and relayed to the government with the number of homes needed. Then, one lump sum to catch up on the number of houses needed, rather than incremental investments.
Isfeld said he’s seen the government take too slow of an approach in communities, or focus on one community in deep trouble, to try and set a phony example. Isfeld wants a change.
“People have to look at this more as a black and white situation,” he said. “Never mind the grey areas, people’s lives are at stake—children’s lives are at stake. And they play politics with it all the time.
“And addressing one community, just one community alone, then puffing your chests out like the politicians they are and take credit for doing something grand—because they did nothing, they did nothing but put a band-aid on a festering situation.”
Dayne Patterson is a recent graduate from the master of journalism program at the University of King’s College in Nova Scotia. He was born and raised in the Canadian prairies, and currently lives in Saskatoon. He would like to thank University of King’s College journalism professor Fred Vallance-Jones for his assistance with this story.
How the By the Numbers story came about
I remembered how past viruses—H1N1, SARS—had affected the First Nation population in Canada. To find out how Covid-19 might be doing the same, I looked for case numbers and population data.
I started looking in December. I checked the Indigenous population in provinces such as Saskatchewan and Manitoba, and used Statistics Canada data to estimate how many Indigenous people lived in reserve communities. Then, I compared the rate of infection in the general population, as posted by government Canada—they didn’t post those rates specific to First Nation communities.
That fall and winter was when Covid-19 entered First Nation communities. The data I found, and my initial calculations with approximate population, showed that infection rates in First Nation communities were at least double the rate of the general population in Saskatchewan, and slightly higher in Manitoba.
In January, I started tracking the case numbers.
Several days a week, Indigenous Services Canada updates the total number of COVID-19 infections on First Nation reserves in Canada. Unlike the government of Canada COVID-19 updates, the ISC doesn’t show the actual number of cases for a day, the rate of growth, or per capita rates —only the cumulative number of cases to that day for First Nations in each province, and the number of active cases, hospitalizations and recovered cases for all First Nations in Canada.
The department also publishes an Epidemiological summary showing weekly trends.
I have been collecting the Covid-19 data posted by ISC nearly every day since early January.
By using the case data from ISC, and the department’s data on registered First Nations populations as of February 2021, I calculated the approximate rate of total cumulative cases for First Nation people living in on-reserve communities. The COVID-19 cases posted by ISC don’t include those who live off reserve or in the territories.
When I compared with the general population data from provinces in Western Canada, the rates of total cases for 100,000 in First Nations were sometimes more than twice that in the overall population. Rates are lower than in the general population in eastern Canada, but with 61 per cent of the registered First Nations population in the west, it has a huge influence on the overall picture.
There are limitations to this analysis and the data used. While the registered population data for First Nations is the best available for calculating provincial rates, it may not be completely precise as it doesn’t include people who are entitled to register as status Indians but don’t, or whose registration hasn’t been confirmed.
For example: a newborn baby may not be included on the list; a recently deceased person may have not been removed from the list; or a person may choose not to document their community of residence.
There is also a small difference in the timing of the population data used to calculate rates per 100,000 on First Nations and in the general population. The registered First Nations populations data is from February 2021, while the data for the general population uses population data for the third quarter of 2019.
For all these reasons, the rates on First Nations and the calculated differences with the overall population should be considered approximations based on the best available data.