A First Nations woman who lives in Whitehorse is speaking out against the territory’s lack of services for dialysis patients.
Nellie Njootli, 29, is a Vuntut Gwitchin First Nation citizen and has been living in Vancouver for the past six months for treatment.
At age nine her kidneys began failing and she was diagnosed with End Stage Renal Disease (ERSD) and Chronic Kidney Disease.
Njootli’s diagnosis did not require her to undergo dialysis, a procedure to remove waste products and excess fluid from the blood when the kidneys stop working properly. Soon after she received a kidney transplant and her life went on as usual.
But in May, 20 years after her transplant, doctors discovered she had kidney rejection and Njootli was once again diagnosed with ERSD. Her situation is treatable – but Njootli had to move to Vancouver for help.
“I was brought to emerge (Emergency), wheeled upstairs, and I got my central line put in into my chest and dialysis was started right away. I have been on dialysis since,” she told APTN News.
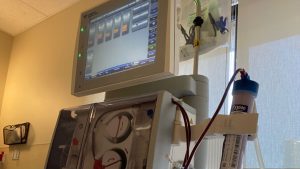
Three times a week Njootli undergoes hemodialysis, a dialysis treatment which is administered through a machine, typically in a hospital setting.
But Njootli said she’s unable to return home to Whitehorse because hemodialysis is not offered in a hospital setting in Yukon.
Non-insured health benefits for First Nations and Inuit pays for Njootli’s accommodation in Vancouver and provides her with a small allowance for meals.
Njootli said she still pays for her apartment in Whitehorse and that her meal allowance doesn’t always cover the cost of groceries.
She said she’s burning through her savings in order to cover her expenses, an issue she wouldn’t have if she could receive hemodialysis in Whitehorse.
“I personally think that the lack of a dialysis center in the Yukon is long overdue and very baffling,” she said.
“My mom told me that when I was younger, she was very hopeful that surely there would be (hemodialysis) by the time I would need a new kidney. But here we are two decades later and nothing has changed.”
Njootli said she is also struggling with being away from home for an extended period of time.
“People want to be near home, near their support networks, near their friends and family when they’re going through a health crisis.”
Gaps in the system
According to the Canadian Institute for Health Information, compared with other Canadians, First Nations, Inuit and Métis people are four times more likely to travel long distances (over 250 kilometers) for treatment because kidney care services “are not delivered in a geographically appropriate way.”
Anne Huang, who is on the board of directors for is The Kidney Foundation of Canada, B.C. and Yukon Branch, said Njootli’s experience isn’t uncommon in Yukon.
“It’s really tough having to fly down to Vancouver and some people have to live there because you have to do hemodialysis three times a week sometimes,” she said.
Huang said the board is supportive of establishing a hemodialysis unit in Whitehorse but she said only a small number of people are undergoing dialysis in the territory at any given time.
“The main obstacle to getting an in-territory unit is that we don’t have enough people who are in need of dialysis right now to justify the cost,” she said.
Read more:
‘I had to give a piece of myself to get my dad home’
White Dog First Nation man on ‘dialysis strike’ until band changes
Ken Hegan, a communications analyst with Yukon Department of Health and Social Services, said BC Renal supports patients in Yukon who need dialysis or a kidney transplant.
“Their guidelines do not recommend developing a hemodialysis centre in the Yukon based on a number of factors, including the territory’s population and the number of Yukoners who would need the service,” he said.
“Over the past five years, the number of Yukon patients needing dialysis was 10 or less, and did not meet threshold guidelines for the development of a local hemodialysis unit.”
Hegan said a population of 85,000 would require 24 patients as a base requirement for a community dialysis unit. A unit would also need a resident nephrologist or internist and three to four specialized nurses.
“Even if a centre were created, some patients would still be required to relocate out of territory for hemodialysis due to complex or advanced needs,” he said.
Hegan noted there are currently less than five patients in need of full-time hospital dialysis. He said they can be supported by the Medical Travel program for long-term treatment in BC.
He said 10 people in the territory are currently undergoing dialysis treatment at home through either peritoneal dialysis, a less restrictive form of dialysis that requires a patient to have a catheter placed in their stomach, or home hemodialysis where patients can administer their own care at home.
Hegan added a review completed by the Canadian Agency for Drugs and Technologies in Health in 2017 found independent dialysis, such as peritoneal dialysis and home hemodialysis, are as effective as hemodialysis provided in hospital settings and is the preferred first option for patients.
Huang said while The Kidney Foundation is also lobbying for home hemodialysis, it might not be for everyone.
She noted patients in Yukon who choose home-based dialysis are required to undergo two months of training in Vancouver. As large fluid-filled bags are also required for home dialysis, Huang said it’s optimal for patients to have an adequate amount of storage space.
“If you don’t have enough space for a month’s worth of fluids to store then it’s very impractical,” Huang said.
Njootli agreed.
She doesn’t feel home dialysis would a suitable option for her as the treatment would entail the dialysis machine to be connected to her apartment’s water supply, something she’s unable to do as a renter.
Njootli noted it would also require her to act as her own nurse, something she’s not comfortable with as she lives alone and has low vision.
Njootli said ultimately, it’s up to the territorial government to make in-territory hemodialysis treatment a priority.
“I would say that when there’s a will there’s a way, and I believe in our healthcare system to find a way to fill that need and fill that gap,” she said.
‘A new lease on life’

Njootli said she’s been approved for peritoneal dialysis. Though she’s anxious about having a tube placed in her stomach, she said if all goes well after she receives the catheter placement she could be home by the spring.
In the meantime, she’s appealing to the public to help her improve her quality of life. She recently created a website sharing her story in hopes of finding a living donor and to raise awareness about kidney donation.
Njootli said receiving a kidney from a living donor would be the best option for her as the kidneys typically last longer and there’s more time taken to ensure a match.
So far, a handful of people have expressed interest – mostly strangers – which she’s grateful for.
“For me, receiving a kidney would be incredibly life changing. It would equal a (new) lease on life. I’m not even 30 yet. I’ve got so many things I have yet to accomplish and want to accomplish,” she said.
“Receiving a kidney would be equal to receiving hope.”









